Handle with care

Until my 28th week of pregnancy, I had been the […]
Until my 28th week of pregnancy, I had been the ideal prenatal patient: appropriate weight gain, moderate exercise, healthy eating habits, and normal test results. But during my routine checkup that first week of my last trimester, my doctor discovered that my stomach measured smaller than it had four weeks earlier.
My doctor—and the doctors I saw subsequently—speculated about many things: low amniotic fluid, slightly elevated levels of protein in my urine, sluggish fetal growth. With nothing conclusive, I went on bed rest as a precaution with my doctor assuring me she was going to remain vigilant about my health.
Several weeks later, my body went into complete shutdown mode. It was only then that my doctor realized I had HELLP Syndrome, a dangerous variation of preeclampsia. Twelve hours after my diagnosis, I gave birth to my 4-pound daughter. With her birth, the dreams I had of my perfect delivery vanished. Instead of holding our newborn, my husband and I watched as nurses wheeled our preemie into the neonatal intensive care unit (NICU), where she would spend her first 10 days of life.
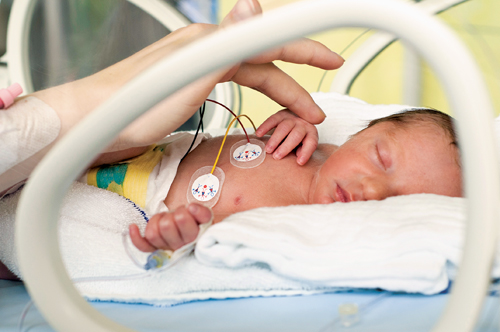
Most mothers-to-be know the risk factors for having a NICU baby. But no matter what precautions are taken, a baby’s needs are often unpredictable. Having a premature baby was not something I thought would happen to me, and I definitely never imagined my firstborn would be staying in the NICU while I went home.
While the number of preterm babies born in the U.S. fell for the sixth consecutive year in 2012, according to the National Center for Health Statics, prematurity is just one reason a baby may need to spend time in the NICU. Other reasons for a NICU stay include maternal stress, such as pre-eclampsia, a difficult delivery, or special circumstances with the baby, such as birth defects or respiratory issues.
Liza Cooper, director of family-centered care and family engagement for the March of Dimes in New York City, says that for any mom who is in labor, a baby’s stay in the NICU is always a possibility. Moreover, she says, it’s usually a surprise.
Whether anticipated or unexpected, having a baby in the NICU can be a stressful time, and it’s important to be ready, just in case.
Always be prepared
Regardless of risk for delivering a NICU baby, Cooper says it’s wise to arrive at the hospital as informed as possible. “The more informed the parent is beforehand, the better she’ll be able to advocate for her baby if, in fact, he does need to go into the NICU.”
When Ambrosia Sauer, a mother of four in Center Grove, Indiana, became pregnant with triplets, she knew right away that a NICU visit was a distinct possibility. “Lots of multiples have to spend time in the NICU, and we knew we needed to prepare,” Sauer said. “As part of a class my husband and I took a class called ‘Multiple Blessings,’ we toured the NICU. We got to walk through it and ask questions about it. I also read as many books as possible to educate myself about what the birth of my babies might look like.”
But for a majority of parents whose babies wind up in the NICU, there is no such preparation. Kelly Spears, RN, from Indianapolis, Indiana, says that the majority of babies that visit the NICU do so as a result of preterm labor or an immediate issue after delivery. “Most of our preterm babies come as a result of preeclampsia or HELLP syndrome, and their babies go to the NICU as what we call ‘feeders and growers,’ babies who need a little extra attention at the beginning,” she said. “Then there are babies who, for whatever reason, are not transitioning well once they’re born and need to go to the NICU for observation.”
Remember, she says, that while in the NICU, your baby is going to get the undivided attention of a specially trained staff.
All in due time
Just as the reasons babies need to go to the NICU are varied, so too is the length of their stay. Some babies may only need a few hours of special observation, while others, like Sauer’s babies, need a month or so to feed and grow. In extreme cases, babies may need several months of NICU care prior to being released to their parents.
The length of stay in the NICU varies by baby and level of difficulty, but it’s an experience that bonds parents who have gone through it. “As one mom told me,” Cooper recalls, “‘If you’ve left your baby in the NICU even for an hour, you’re part of the club.’ You know what it’s like to be separate.”
Join the team
Sauer’s babies ended up being in the NICU for nearly a month, which meant the bonding process between mother and children shifted out of necessity. Cooper says when such stumbling blocks arise, it’s critical for mothers and fathers to become active members of the NICU. “It’s very important that moms and dads feel highly involved with the care of their baby,” she says.
Get to know the nursing staff
“When your baby is in the NICU, she is going to receive care from the nurses … not their mothers,” explains Spears. As a result of this focused care, the staff will know a lot more about your baby than even the on-duty physician. If you become concerned about your baby’s progress or don’t fully understand what is going on, don’t be afraid to ask questions, Spears encourages. “When things happened I didn’t understand, I asked a lot of questions,” Sauer recalls. “The nurses were wonderful. They were patient with me and all my questions, and they always were happy to explain what was going on with my babies.”
Bond the best way possible
“Especially if a baby is a ‘feeder and grower,’ parents might not get to hold him right away in the NICU,” Spears said. When that delay occurs, Cooper says, it is normal for parents to grieve what they imagined the delivery to be. It’s also normal still want to bond with your baby, despite the situation.”
For Sauer, who worried about bonding with her triplets, one solution was to pump her breast milk. “Since I wasn’t allowed to hold them very often or interact with them as much as I wanted to, pumping breast milk for [my babies] was one way for me to care for them like I would if they were with me,” she explains. While she did mourn the reality that she would not be able to nurse the triplets, as she had her first child, “Pumping gave me a purpose,” she says. “[It was] something active I could do to help the babies even when I couldn’t be with them.”
In addition to pumping, Cooper suggests that moms advocate for themselves and their babies by engaging in kangaroo care with their NICU babies. Kangaroo care, in which parents hold their baby for skin-to-skin contact, should be encouraged and supported as early and as often as possible.
“The research on kangaroo care shows enormous benefits to the mother and father, as well as the baby. It is beneficial in terms of bonding, breast milk production, the baby’s growth, respiration, and even the baby’s ability to tolerate discomfort. As soon as it’s safe for the baby to be held, moms and dads should ask about kangaroo care.”
Home alone
Some moms will need to deal with the reality of going home before baby has been released. When Sauer was released four days after delivery, she knew her triplet sons would not be going with her.
“When we got to the house, and the babies weren’t with me, I just remember how silent the house felt. The nurses had sent me home with pictures of the boys, and that helped. But it was still a very lonely time,” she said.
Such feelings are common, Cooper says, and sitting with the uncertainty is normal. “The best advice I can give is to be honest about your feelings, to talk about what’s going on with someone who is very supportive—a partner, a best friend, a nurse, or even other NICU parents online,” advises Cooper.
Sauer agrees: “Having my friends come and visit me was a huge help, and I’d encourage all NICU moms to reach out to as many networks as they can, especially early on.” Ultimately, Cooper suggests, the most important things to remember are that your baby is getting the best care possible and that by leaving her in the NICU, you are being the best advocate possible.
Going home without her babies triggered many emotions, admits Sauer, including guilt, anger, and inadequacy. But in the end, she realized she was being the best mom she could be by staying involved in the NICU care of her triplets. “Even though the experience of having my babies in the NICU was hard, the staff was wonderful, and I knew they were receiving the best care possible.”







