All in a day's work: The birth of Grayson
Let’s start at my 35th week. (Let it be noted that […]
Let’s start at my 35th week. (Let it be noted that while all of this was happening, I had a bad case of bronchitis, an upper respiratory infection and a sinus infection!) We went in for my checkup and did the basics—weight, blood pressure, etc.—and then I had to sign some paperwork saying if such and such happens, I want them to do this or that, and in case of emergencies, they can do this and that … blah blah blah. Then my doctor checked for the first time to see if I had dilated at all. It turned out I was already at 3 centimeters. That’s 3 centimeters less that I would have to labor through—WIN!
Then it was time to ask questions … I asked my doctor if I had possibly been experiencing Braxton Hicks contractions, as I’d been feeling my stomach tightening but had felt no pain. She responded, “Is it all over the stomach, or just the right side?” It was just the right side. “Then it’s probably just him pushing his butt up, since it’s not over your entire stomach. You’ll know the difference when it comes to it.”
And that was that.
With week 35 begin the weekly appointments, instead of every two or three weeks like they’d been. My doctor told me she wouldn’t be available next week because she’d be on call at the hospital, but I would see her associate for that appointment.
The day before the appointment, I found out that Jon had a meeting at work and couldn’t come with me. (He had come to every single appointment.) So now it was not just a new doctor, but I also had to go alone. Seriously?
The morning of my appointment, I logged into my account at the clinic and was looking through my medical history. I noticed that my blood pressure had been going up just slightly throughout my entire pregnancy, and I mentioned this to my best friend—we like to worry about things together, and blood pressure had been a topic of discussion on multiple past occasions.
When I got to the clinic, the nurse took my blood pressure. At 140/70 it wasn’t super high, but I immediately made a mental note of this because it had been on my mind all morning. The doctor came in to tell me I was still at 3 centimeters (dang!). Before I had a chance to ask her, she said she wanted to check my protein levels due to my slightly elevated blood pressure. She sent me over to the lab and said she’d call me as soon as she had the results. I chalked this up to me being nervous about seeing a new doctor without Jon, and I actually didn’t worry about it at all.
As soon as I got home, she called me back. The normal level for proteins should be under .3, and mine were at .8. She wanted me to head to the hospital RIGHT AWAY for a 24-hour urine test. This meant I’d have to put all of my urine into a jug on ice for a full 24 hours, so they could count my proteins and find a more conclusive result.
Jon and I headed to the hospital straight from his office and got there right after 5 p.m. At the birthing center, I told them I had been sent over from the clinic and that they should have my information on file already. Then they asked me if I was being admitted. I didn’t know. I didn’t think so? I thought I was just coming to get a jug to pee in.
They put me in a room to monitor me and see what was going on … and had me pee in yet another cup. That cup came back with a protein level of .11. The number just kept rising. I was told that I would be admitted, spend the night and, who knows, maybe even have the baby that night.
Wait … WHAT?!
They thought I might have preeclampsia but still wanted to do the 24-hour test to make sure. I thought I would just be peeing in a jug all night—not birthing a child!
We were not prepared for this at all. We had no bags packed—and I don’t mean that we didn’t have them with us, I mean I hadn’t gotten around to packing my hospital bag yet, and the nursery was a complete mess. We hadn’t even picked a name. (I had my favorites, but Jon was pretty sure he had plenty of time!)
The next morning, they told Jon to go to work as there would be no use in him worrying and doing nothing with me all day—and I would be there until at least 8 p.m. waiting for the test results to come back.
When I first got pregnant, I prepared myself that this baby might have a large head—it runs in the Henderson side of the family. I cannot find a winter hat that covers my ears. Where am I going with this? When they took me down for an ultrasound the next morning, the tech said, “Jeez. They may not allow you have this baby naturally. His head is already measuring at 10 centimeters, and it will continue to grow. They may make you have a C-section.” Hey, sure, let’s add this to my list of worries.
They hooked me up to all these monitors to track my heart rate and my baby’s heart, as well as a machine to check for contractions. Guess what? I was having contractions (and not Braxton Hicks contractions). The nurse couldn’t believe that I wasn’t feeling anything because they were registering off the charts—literally. She told me she thought that I would have the baby that day or the next, regardless of the test results. The thing is, I was not feeling a thing. I could feel my stomach tightening, but there was no pain at all.
Tests continued throughout the night. Every time I ate or sat up, my blood pressure would go up. If I reclined, it would be low—they couldn’t figure it out. Jon had to run home at 10 p.m. to get a bag of necessities for us and make some calls (just in case we did have a kid by morning), but he was freaking out because he didn’t want to leave and have something happen to me while he was gone.
The next morning, my OB showed up to say she had good news and bad news. The bad news? I had mild preeclampsia. The good news? I was having a baby on Tuesday. They wanted to wait until 37 weeks for him to be what they consider full-term. I was just over 36 weeks, and Tuesday would make 37. I would have to come back on Sunday for them to rerun all of these tests, and then check in bright and early Tuesday morning to be induced.
Time to cancel that baby shower my sister-in-law and niece were throwing for me (in another town) the next day.
My doctor was an integrative doctor; she was all about doing things holistically and naturally. She had my back the entire time about wanting a natural birth with no drugs and loved that I wanted to do this. Then she said this: Because of the PE, I would have to be on a magnesium drip to prevent me from having seizures. This would limit my mobility because it would make me nauseous, which would mean no walking the hallways to speed up labor. Because I would be induced, contractions would be full-force from the start, and my body wouldn’t have a chance to build up a tolerance. To our disappointment, she said I would more than likely want an epidural. She said to expect 20 or more hours of HARD labor, and she seemed even more bummed about the birth plan being altered than I was. Because she wouldn’t be on call that day, she wouldn’t be delivering my baby, either.
While Jon was gone, they hooked me up to the Pitocin and got the day started. Then I waited for the intense pain to begin. Jon got back to the room at about 10 a.m. I was at 4 centimeters but still felt no pain. The nurse was amazed. Women in the rooms around me were screaming bloody murder while I sat there texting all my family and friends, watching TV and just taking a few deep breaths to help myself relax. The doctor and resident came in at 11:30 a.m. to say they were going to break my water and that they highly suggested I get an epidural—the contractions would become very painful, and once they broke the water I couldn’t get one.
I didn’t have a birth plan for a natural delivery just to prove that I was some strong woman who didn’t need medication; I had nothing to prove to anyone. I wanted to be able to have that experience, and I also didn’t want a giant needle shoved into my spine. In the end, I went with the epidural. It would be in my control, so I wouldn’t need any medicine if I didn’t want it, but I could hit the button to give myself some relief if the pain got too intense. Ten minutes later, the anesthesiologist walked in. (Jon had to leave because it’s a sterile procedure.) She watched the monitor for my contractions and said, “Wow, you’re going to be a great mom if you’re this calm through that contraction. Are you sure you even need this?”
Just as she inserted the tube, the door to my room opened. Remember how I said this was a sterile procedure? The birthing center was under construction and was updating its rooms by putting in whirlpool tubs and new countertops. So this person who walked in … yup, it was the construction crew coming to vacuum out the bathroom vents. OK. It was dumb that they didn’t have a sign on the door for a procedure in progress (seriously, what if I had been delivering the baby right then?!), but why wouldn’t they knock?
Twenty minutes later I was numb from the waist down from the initial test-drip in the epidural, but it wasn’t as bad as I thought it would be. I could still feel my legs enough to move them. The doctor walked in and broke my water right at noon, but I was still only at 4 centimeters. They checked me again at 1 p.m. and BAM, 10 centimeters, just like that.
They wanted me to rest a little because I had quite a few hours of pushing ahead of me. The rest would allow my baby to move further down, so I wouldn’t have to work as hard during the delivery. My awesome nurse left at 3 p.m., and a new nurse came in and said, “Oh, you’ll definitely be eating dinner tonight!” (Dinner stops being delivered at 7 p.m.) She said she was going to have me use the “peanut,” which is like an exercise ball. She put it between my legs and had me lay on my side and said, “Let me know if you feel like you need to poop because that’s your body wanting to push.” So I went about my texting and TV-watching. My mom was waiting by the phone anxious for news, my best friend was crying at work all day waiting for news, and Jon’s co-workers were texting him for updates. I took a little nap.
The nurse woke me up to ask if I felt like I needed to poop yet. I told her that I didn’t, but that I felt like his head was RIGHT THERE whenever I felt a contraction (which was still just a tightening of the stomach).

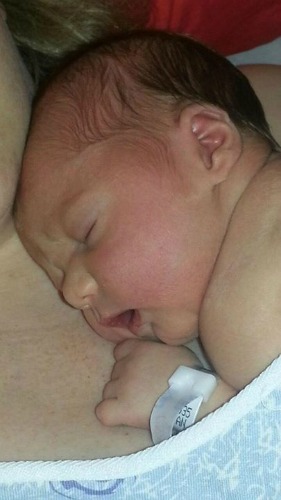
After a practice push, she hollered for the full delivery staff. At 5 p.m. exactly, they told me to start pushing (three pushes of 10 seconds during each contraction). Six and a half contractions and 19 minutes later, our little guy arrived. I thought for sure he hadn’t moved at all during the pushing, but before I knew it he was on my chest and immediately peeing all over me.
I looked at the doctor, who was stitching me up. “That wasn’t bad at all. I could do that again right now!” Then it hit me. My right ear completely lost its hearing, and I felt so nauseous that I couldn’t think straight. I started pointing at my ear and sort of hitting that side of my head, not knowing how to put what I felt into words. They could tell I was fading fast, and the resident started yelling at me to keep talking to her. I started puking in a bucket.
Grayson was thrown at Jon as my blood pressure dropped to 60/30. They couldn’t figure out why—this only happens with major blood loss. Nurses that have been there for more than 40 years had never seen this happen before, and my blood pressure was not improving. The doctor shouted to give me a shot of ephedrine, which helped for a minute or so before my blood pressure dropped again. A second shot was given, and my blood pressure seemed to hold steady. It took them about an hour to get me stitched up, and then I finally got to hold and nurse the baby I had been waiting nearly six long years for.
I was unable to sit up for 36 hours because my blood pressure would drop, and I would almost pass out every time I tried. Doctors came in at 3 a.m. and gave me an EKG—everything came back A-OK. I had no more bleeding than any other woman who had just given birth, but my hemoglobin was ridiculously low. They ended up having to give me two blood transfusions, but they had no idea what caused the issue even after all the tests were run.
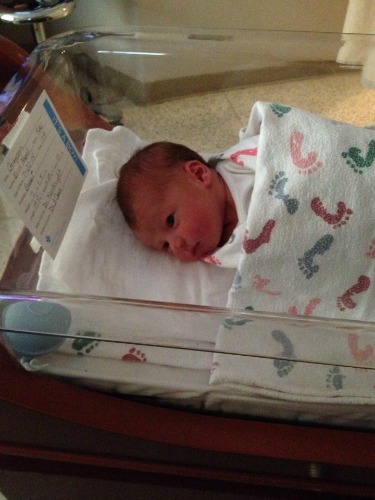
Poor Jon! Our hospital no longer had a nursery, so the baby stays with you the entire time you’re in the hospital. With me unable to move, Jon had to do all of the diaper-changing until I was able to sit up again (and we all know how awesome those first few diapers are). All I could do was lie in that uncomfortable bed, move up an inch every hour (hoping that my blood pressure would steady) and nurse Grayson every two hours. I really shouldn’t complain about that bed too much, though, because I’m sure it was much better than the fold-out chair that Jon got.
So, my labor was literally all in a day’s work—it was from 9 a.m. to 5 p.m., and I still have NO clue what a contraction feels like.
Send us your birth story! Whether you had a home birth, hospital birth, 37-hour labor or emergency C-section, we’d love to read the tale of your little one’s grand entrance. Write up your birth story (click here for tips on getting started) and email it, along with a few photos, to birthstory@pnmag.com. We’ll share it on our Birth Day blog and may even print it in an upcoming issue!







