Types of Prenatal Testing
Peeing on a stick is just the beginning—here’s what’s to come.
Medical Expert: Robin Blumer, MD
Congratulations! The results are in, and you have a budding babe on the way. But that’s only the beginning of the tests you have to take …
If you’re pregnant, get ready to be the center of some major medical attention. There will be a lot of tests (more than you took in high school!), and you’ll clock serious face-time with your health care provider. But don’t worry, all of this poking and prodding doesn’t necessarily mean that there’s something wrong. An onslaught of prenatal screening tests and checkups is the norm for pregnant people, and it’s all to make sure you and your little one are in tip-top shape.
Prenatal testing gives your practitioner insight into how you and baby are faring throughout the pregnancy, and in the case of genetic testing, it can also indicate if baby is showing signs of possible birth defects or chromosomal abnormalities.
But not every prenatal test may be necessary. Here are the most common prenatal tests, why they’re important, and what you can learn from them.
Routine Tests
Your first visit to your doctor or midwife will include a physical exam and a stack of paperwork to go over your family history, current health conditions, and risk factors. You’ll also have to take a urine and blood test. These standard tests will look for issues that could affect your pregnancy like infections, STDs, anemia, and diabetes.
Speaking of urine tests, get used to peeing in a cup because you’ll be doing it frequently throughout your pregnancy. A urinalysis tells your practitioner if you’re fighting off an infection, have high glucose levels (an indicator of gestational diabetes), or are at higher risk of preeclampsia, a serious issue during pregnancy that causes high blood pressure.
Besides multiple urinalysis tests, another blood sample will be taken between 15 and 20 weeks later in pregnancy to double-check that everything’s going well. Additionally, there are also two more tests you’ll receive in the later stages of pregnancy:
Glucose screening and glucose tolerance test, 24 to 28 weeks
This test gets a lot of flack because, well, it’s not enjoyable. After a period of fasting (usually overnight with an early morning appointment) you’ll arrive at your visit (hungry) and be given a drink packed with glucose. This drink is often bright orange or red, though recently clear, dye-free options have become available. It tastes like it looks—like syrup and chemicals; it’s not a walk in the park to get it down, but it’s necessary. (Pro Tip: If you down it really quickly and have a nurse willing to chant “chug chug chug” while you do it, it feels more like a drinking game.)
One hour after consumption your blood will be drawn to check your glucose levels. Some practices may also let you take the drink home and be ready to test upon arrival of your scheduled visit. If the initial screening shows a higher-than-normal result, you’ll be asked to come in again for a more in-depth test called the glucose tolerance test. This three-hour procedure requires you to fast and have your blood drawn before—and multiple times after—downing another bottle of that saccharine drink. The results will indicate whether you have gestational diabetes or high blood sugar during pregnancy.
Group B strep screening (GBS), 35 to 37 weeks
Your OB will swab your vagina and rectum to test for a type of bacteria that many pregnant women carry. The bacteria can be passed to your baby during vaginal delivery, and although it causes you no symptoms and doesn’t affect a majority of babies, it can cause some newborns to become sick. If you test positive for the bacteria, you’ll receive antibiotics at the start of labor. If you go into labor before you can receive the test, you’ll be treated for GBS as a precaution.
Genetic Testing
Early in your pregnancy, you’ll be given the option of undergoing screening tests to look for genetic disorders. The screenings search for certain abnormalities, and the results are an estimate of whether your baby is at increased risk for the associated medical conditions, such as aneuploidy, trisomy, monosomy, and inherited disorders including sickle cell disease, cystic fibrosis, Tay-Sachs disease, and others. Whether you move forward with genetic screening is entirely up to you, but know the results are not certain and should not be used as the basis for making medical decisions surrounding your pregnancy.
Earlier this year, the Food and Drug Administration (FDA) issued a statement warning the public of the risks and potential false results obtained through noninvasive prenatal screening tests (NIPS).
“While genetic non-invasive prenatal screening tests are widely used today, these tests have not been reviewed by the FDA and may be making claims about their performance and use that are not based on sound science,” said Jeff Shuren, MD, JD, director of the FDA’s Center for Devices and Radiological Health in the statement. “Without a proper understanding of how these tests should be used, people may make inappropriate health care decisions regarding their pregnancy. We strongly urge patients to discuss the benefits and risks of these tests with a genetic counselor or other health care provider prior to making decisions based on the results of these tests.”
If you’re newly pregnant and concerned, know that your provider is there to answer all your questions and that you have the right to decline these tests if desired. Remember, too, that these are screening tests—not diagnostic tests—meaning they can only provide information about the risk that a fetus may have a genetic abnormality. A positive result should be investigated further with additional testing to obtain an accurate result.
“Genetic screening tests are intentionally set with a very high false positive rate because they are trying to catch all the possibilities, and then weed through them with an additional test,” cautions Robin Blumer, MD, OB-GYN in Michigan. “Screening tests never make a diagnosis. They simply identify enough reason to offer diagnostic testing.”
If you decide to utilize genetic screening, these are the test you can anticipate:
Carrier screening, preconception to 12 weeks
Based on your background, you may be offered genetic screening for a single disorder like cystic fibrosis, sickle cell disease, or Tay-Sachs disease. These disorders are passed down from parents and are more common in certain ethnic groups. Blood drawn from each parent is needed to evaluate the chance of a baby inheriting one of these diseases. This screening can also be done during pregnancy.
Cell-free DNA screening (cfDNA), 10 to 11 weeks
One of the newer screening methods for Down syndrome and two other chromosomal disorders, cfDNA analyzes the particles of your baby’s DNA found floating in your blood. It’s usually offered to high-risk patients (mainly pregnant people aged 35 and up) for whom the results are most accurate. This test can also tell the gender of the baby well before the 20-week ultrasound for parents wanting to find out before the birth.
First-trimester screening, 11 to 14 weeks
This screening requires both a blood draw and a specialized ultrasound (to analyze folds in your baby’s neck) between weeks 11 and 14. Those two tests, combined with your age, are used to determine the likelihood that your child has a genetic disorder like Down syndrome.
Triple/quad screening, 16 to 20 weeks
This test also looks for genetic disorders. It’s performed using one blood sample drawn between weeks 16 and 18. The triple screen looks at two hormones and a protein found in your blood. The quad screen looks at those as well as an additional protein.
Integrated screening, 11 to 18 weeks
This best-of-both-worlds screening combines the first-trimester screening and the quad screening to give you the highest possible detection of Down syndrome and trisomy 18, along with the ability to identify possible neural tube defects like spina bifida. In total, it requires two blood draws—one in your first trimester and one in your early second trimester, along with a specialized ultrasound.
Diagnostic Tests
If you receive a positive result from one of the screenings, try not to stress. “It’s more convincing that there is a problem if you see evidence of a major abnormality on a good ultrasound or the more definitive diagnostic tests than on a screening,” explains Dr. Blumer.
Think of a screening as the first step in evaluating your child’s likelihood of having a genetic condition. After a positive screening result, the next step is talking to a genetic counselor and determining if you’d like to have a diagnostic test performed.
Depending on your stage of pregnancy, you will be offered the following tests, both of which search for further evidence of genetic disorders and birth defects by evaluating cells from your baby found in surrounding matter:
Chorionic villus sampling (CVS), 10 to 13 weeks
A needle is inserted into the abdomen or cervix to remove a small piece of placenta tissue for analysis.
Amniocentesis, 15 to 20 weeks
A needle is inserted into the abdomen to withdraw a very small amount of amniotic fluid for analysis.
Diagnostic tests offer more concrete results but can also cause miscarriage in a small number of pregnancies. It was previously estimated that 1% of amniocentesis and 1.5% of CVS procedures ended in miscarriage. However, newer research claims that generic figures for the risk of pregnancy loss following these procedures should no longer be used, noting that miscarriage risk following an invasive procedure is very low and that pregnancy loss is likely related to other pregnancy-related and maternal factors.
Like genetic screenings, diagnostic tests are optional. Some parents choose not to have them performed. Others use the diagnostic test results to make health care decisions or prepare for the adjustments a baby born with health problems requires. Weigh the decision with input from your provider and genetic counselor and discuss it with your partner to determine what’s right for you and your family.
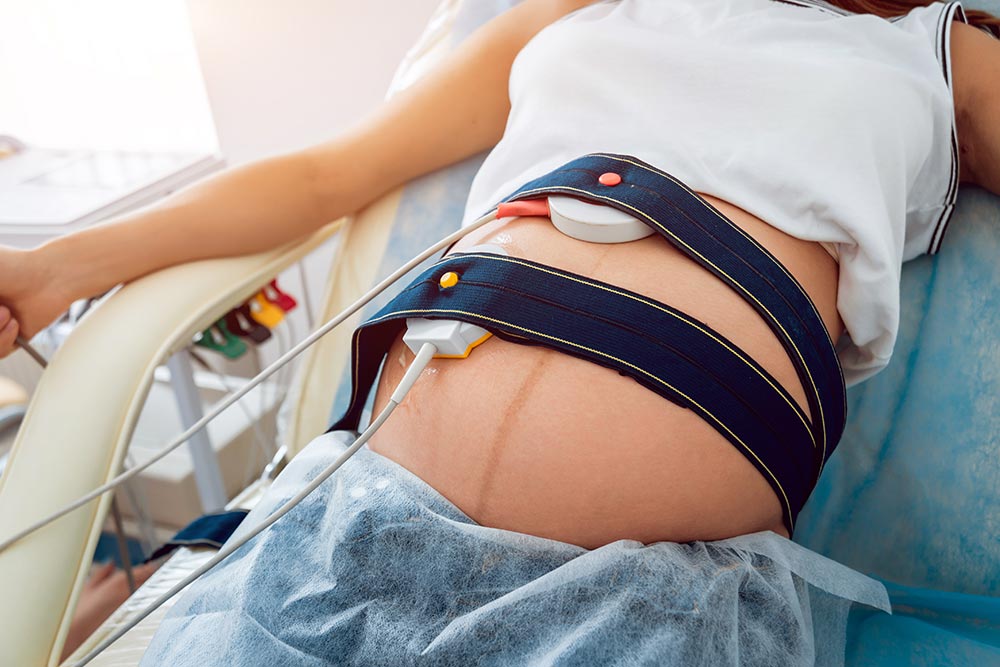
Non-Stress Test
Feeling your little one swim around inside of you is a highlight of pregnancy. But if your baby suddenly seems less active, your practitioner might call for a non-stress test (NST). The NST is a common test primarily used in the third trimester to check a baby’s heart rate and ensure your little one has adequate oxygen. It’s used when a baby has reduced movement or if you’re past your due date, have had complications with previous pregnancies, or have complications with your current pregnancy.
The test requires 20 to 40 minutes of lying down with two belts strapped across your belly. One will track uterine contractions, and the other will monitor your child’s heart rate to see if it changes when they move.
If the results are non-reactive (meaning your baby’s heart rate did not increase with movement), it could simply signal that your child was asleep or inactive. If you’re full-term, your OB might recommend delivery after a non-reactive result. If you’re not full-term, additional tests will follow and may include another NST at a later date, an ultrasound, and/or a stress test that forces a uterine contraction.
Pregnancy is a time of rapid changes, but there’s no need to fret. Your prenatal care team is there to monitor and make sure you and your baby get the best treatment possible, so the excitement of bringing a wee one into the world can remain your primary focus.
This article was originally published in 2016 and has been updated by Lauren Lisle.







