Restrictive behaviors
If you’ll be delivering baby in a hospital, there will likely be some rules and regulations by which you’ll have to abide. There might be a limit to the number of guests you can have in your room, a cap on how loudly you can blast your labor playlist, or a “no candles” policy that snuffs out your tranquil vibe. But you might find yourself restricted in other ways, too—ways that might not be necessary or even helpful.
Free movement
If you’ve seen a big-screen birth, you’re familiar with this scene: Mom on her back in the hospital bed, a nurse pulling back her leg on one side, dad on the other and the doctor down below waiting to “catch” the baby. Hollywood actually (kind of) got this one right. “More often than not, women are confined to bed during the birthing practice these days,” says Robin Elise Weiss, president of Lamaze International. But, she adds, “Lying on your back is not the only way to give birth.”
In fact, it may not even be the best way. Research shows that movement during labor can be highly beneficial for the mom-to-be. Despite this, many women find themselves bed-bound, thanks to policies, procedures and interventions that limit movement.
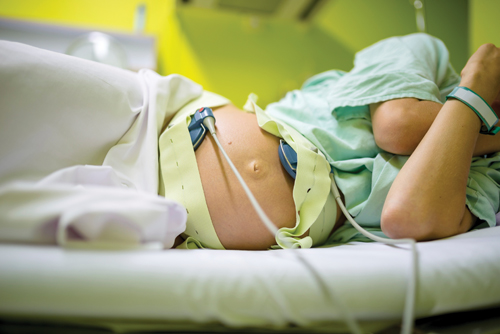
In many facilities, medical intervention from the outset is routine. As soon as you’re assigned a room, you’ll be hooked up for continuous external fetal monitoring (EFM), an IV line will be inserted, and talk of procedures such as Pitocin to speed things along will begin.
In most cases, though, all these “standard” interventions are optional. If you and your baby are both healthy and your labor is progressing normally, EFM isn’t critical; you could opt for periodical checks of baby’s heartbeat via a Doppler ultrasound instrument instead. IVs are inserted early on as a precaution—and do become necessary when interventions take place—but you can request that an IV be inserted only if it becomes truly necessary or that a heparin lock, which allows easy access to a vein if needed, be used instead. Opting out of procedures to speed up labor’s set course is also acceptable, and doing so can help keep you mobile longer.
And according to Weiss, the longer you’re able to move about, the happier you’ll likely be: “Movement helps speed up the labor process,” she says. It also allows your muscles—including your uterus—to work more efficiently and adjusts the bones of your pelvis to help baby find open space to travel through.
“When moms walk around or change positions in the bed, they can help decrease labor pains and use gravity to help the baby move through the birth canal,” Weiss notes. Catherine Ruhl, CNM, director of women’s health programs at the Association of Women’s Health, Obstetric and Neonatal Nurses in Washington, D.C., agrees: “Upright positions are ideal because then the force of gravity is mobilized.” Movement can also sometimes kick stalled labor into gear.
Walking is the obvious choice for staying active (just observe the halls of any L&D unit for proof), but there are plenty of other ways to maintain motion as well. Bouncing and rocking (either in a chair, on a ball or on your own) allow for rhythmic movement, which can help ease discomfort. Changing positions frequently can provide additional relief. Try squatting, kneeling, lunging, bending over the bed and shifting to all fours. (The latter can be especially helpful if you’re experiencing back pain.)
Even if you do have to climb into bed, try lying on your side rather than on your back. “It’s important to note that when staying in bed is necessary, women can still change position frequently,” says Ruhl. A posture might seem comfortable for a few minutes, and then suddenly become very uncomfortable; keep moving. They don’t call it labor for nothing. It’s a journey, and not one you should necessarily take lying still.
When it’s time to push, continue to explore different stances. Squatting can be particularly advantageous during this time. Listen to your body and push according to its demands, not those of someone holding a stopwatch by your head. Guided pushing can be effective in some cases, but in most instances, a woman can deliver a baby just fine pushing on her own terms—a “delivery director” isn’t always necessary.
Food and drink
You might be asked to abstain from eating and drinking anything other than water while in labor—but this is another practice that’s outdated and typically unnecessary. “It’s OK to eat and drink during labor,” counsels Weiss. “You wouldn’t run a marathon without fueling your body, so why would you go through potentially hours of labor without eating?”
Consumption-related restrictions are often in place due to a fear of possible medical complications. “There were studies done in the 1940s that showed a small risk for women who had fluids or food by mouth during labor to have a … condition called aspiration if they needed general anesthesia for an emergency cesarean,” explains Ruhl.
However, general anesthesia is rarely used in childbirth these days, even for cesarean deliveries, and improved anesthesia practices over the years have lessened the risk of vomiting. In fact, a 2013 research analysis of more than 3,000 women by Cochrane Pregnancy and Childbirth Group found no evidence to support a need for restrictions on eating and drinking during a typical labor.
But abstaining during labor remains the norm. “One recent survey of women who gave birth showed that only 40 percent drank fluids and 20 percent ate food during labor,” says Weiss.
Because having a baby is an exhausting business, don’t be afraid to fuel up. Bring along snacks, such as simple carbohydrates (think bread and crackers) and fruit. In addition to water, Weiss recommends fruit juices and sports drinks for liquid refreshment. Sports gel packs are a good option, too. “They are used by endurance athletes because they are easy to digest and process quickly for a boost of energy,” Weiss says.
What if you’re in the mood for a cheeseburger? You know your body better than anyone else. If fatty foods tend to make you queasy, avoid them. But if you can chow down with the best of them and are craving something substantial, there’s no reason to deny yourself. Although nutritionally beneficial foods are healthier for you, there’s no better time to treat yourself than during labor and delivery.
Ruhl notes that in the case of a high-risk pregnancy, eating and drinking might be off-limits for good reason. However, women without such risk factors may drink and eat what appeals to them. As with all labor and delivery room practices, it’s vital that you communicate with your doctor or midwife and research the practices and policies of the places where you’re considering delivering. Although hospitals have come a long way in making labor more comfortable for moms-to-be, some do have restrictions in place that could leave you bed-bound or “hangry.”
If you can’t find a hospital that will meet your needs, consider looking for a birthing center that might be a little more flexible. And begin delivery discussions with your care provider early in your pregnancy to make sure you’re on the same page. If he’s pro-Pitocin and you’re not, you might not make the best team. You’re in the driver’s seat. Conduct interviews, compile research, and make an informed decision about who will bring your baby into this world and where that will happen. But be sure to leave room for a bit of flexibility as well—because no matter how carefully you plan, baby has the wheel once she gives herself the green light to go.







