What Happens to Baby’s Umbilical Cord After Birth?
What you need to know about this lifeline after you cut the cord.
Expert: Mark Sloan, MD, MPH
You’ve been dreaming about this moment for the last 40 weeks (give or take)—your little one is finally here! But after the hard work of delivery is done and before you bask in newborn bliss, there’s one more piece of the puzzle to contend with: baby’s umbilical cord.
The umbilical cord serves as a lifeline in the womb, so special attention is in order as baby transitions postbirth to their independent self. As such, there’s a lot that new parents need to know about clamping, cutting, and postpartum umbilical cord care—from umbilical cord stump to umbilicus (aka baby’s belly button).
Cord of Life
For eight or so months, the umbilical cord (fully formed at around seven weeks gestation) carries nutrients and oxygen from you to your baby and delivers deoxygenated blood and waste back to the placenta. At full-term, it contains two umbilical arteries and one umbilical vein. On average, it’s around 20 inches long.
After delivery, the cord’s blood vessels are clamped and compressed to stop blood from flowing in either direction. This can occur just after birth, separating the cord from the placenta, as has been standard care in hospital births for decades. According to the American College of Obstetricians and Gynecologists (ACOG), it’s best practice for doctors to clamp the cord between 30 and 60 seconds after birth.
Your doctor or midwife will use two (metal or plastic) clamps to reduce or stop blood from escaping, and then your partner or care provider can cut the umbilical cord between the two clamps. Neither the birthing parent nor baby feel any pain as the cord is cut because, like your ears, it contains no nerves.
Delayed Clamping
Although most Western doctors still clamp the cord within a minute of birth, healthcare providers are taking note of research that suggests baby benefits from delayed cord clamping, or waiting until the cord has stopped pulsating to clamp. Research indicates that the umbilical vein closes slightly later than the umbilical arteries, allowing blood to return to baby in the first few minutes of life, which may offer a healthy boost.
Mark Sloan, MD, MPH, pediatrician and author of Birth Day: A Pediatrician Explores the Science, the History and the Wonder of Childbirth, has written about the benefits of delayed cord clamping. “At term, roughly one-third of a fetus’s blood supply resides in the placenta. In the course of labor and delivery, much of that blood is transfused from the placenta into the newborn, driven by the force of uterine contractions,” he explains. “That transfusion continues beyond the moment of birth; if left undisturbed for one to three minutes, the placenta will deliver about three additional ounces of blood to the newborn.”
Studies have shown that a small amount of additional blood can benefit baby in a number of ways, including providing them with a healthy supply of iron for up to six months, which is essential to baby’s brain growth and development.
If you are interested in waiting to clamp baby’s cord, speak to your healthcare provider about including this request as part of your birth plan. “Most physicians will take a [parent’s] desires into account, and as the benefits of delayed clamping are becoming more widely known, many hospitals are changing to make delayed cord clamping standard care in their labor and delivery units,” Dr. Sloan says.
Cord Blood Banking
If you’ve chosen to collect cord blood to bank for your family or to donate, this occurs between the time the cord is cut and the placenta is delivered. Your healthcare provider retrieves the cord blood sample from the end of the umbilical cord, which attaches to the placenta, while you and your babe bond and remain unbothered.
After the cord blood has been collected in a special bag, it will be processed in a lab before being stored in a facility (this may be public or private, depending on what you choose). This blood can later be used to treat certain diseases, including helping offset the side effects of cancer treatment on the immune system.
Umbilical Cord Stump Care
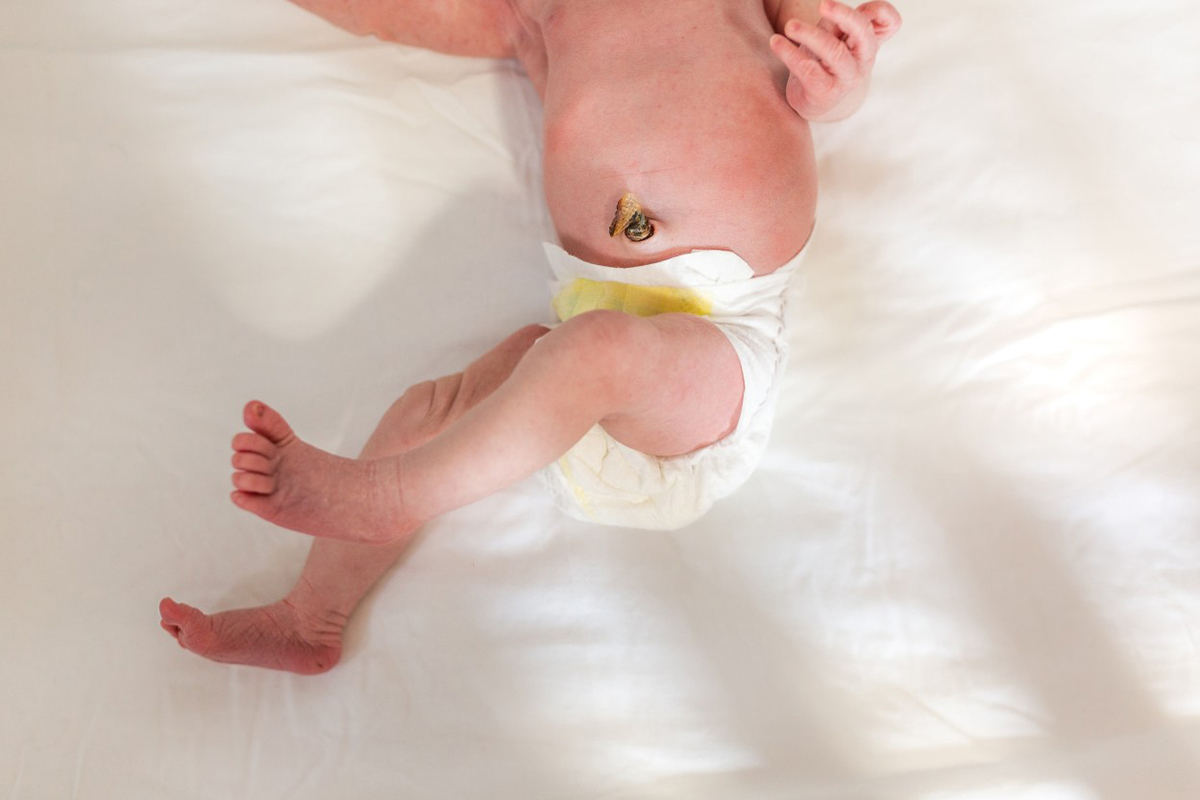
Regardless of whether you delay clamping, once cut, there will be a short cord stump left. According to the American Academy of Pediatrics (AAP), The baby’s umbilical cord stump falls off within a few weeks postbirth and should heal without complications if dry cord care is practiced and left to fall off on its own—no tugging or picking.
Keep it clean and dry as it heals (no rubbing alcohol, which may kill helpful bacteria), and give your baby sponge baths during this time instead of placing them in a tub of water. Dress baby in loose clothing, and fold their diaper down or cut out an opening so it doesn’t rub against the stump, allowing air to help dry it out.
It’s normal to see a few drops of blood on baby’s diaper after the stump falls off (similar to how a scab can bleed a little). However, the AAP notes that if the cord area has a yellowish discharge, you notice redness or swelling around the base of the cord stump, a pink moist bump appears (granuloma), or baby cries when you touch the umbilical cord stump or the skin around it, these may be signs of umbilical cord infection. If the symptoms don’t clear up on their own or the stump hasn’t fallen off after three weeks, reach out promptly to your pediatrician.
It’s truly incredible just how much the umbilical cord does for your baby as it grows and develops in utero. And even the aftercare required after birth is worth it—because your little one will be left with an adorable, tiny little belly button as a result (which is also a reminder of your body’s amazing work).







