A last-minute detour: The birth of Isaac
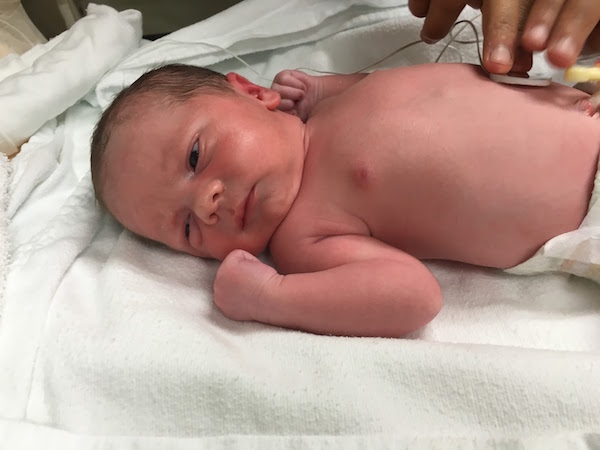
After my daughter, Addy, was born, I had my heart set on a VBAC. I labored very quickly with Addy and pushed hard for two hours to have her head still stuck at -1 station. When she was delivered via C-section, her head was crooked. The doctor said her head was tilted toward one shoulder, so it wasn’t coming through straight on. I was pretty disappointed at being so close yet so far from a vaginal delivery, and I got the baby blues pretty badly in the hospital. I was overwhelmed with the recovery, and the hormones weren’t helping either.
This time, my doctor and I decided to try for a VBAC if I went into labor naturally before my due date. We scheduled a C-section for the day after my due date (September 29).
On Monday, September 19, I had just carried several loads of groceries up the giant stairs to our apartment, and I put Addy down for quiet time. It was after 1 p.m. As soon as I closed my eyes to squeeze in a nap myself, I felt a contraction. After 90 minutes of contractions nine minutes apart, I called the doctor.
I had been in the office that morning and was 4 centimeters dilated and 70 percent effaced, with a bulging bag of waters. The nurse said, “No, we usually wait until contractions are five minutes apart—wait, no, the doctor says to come in because your labor will go quickly.”
I called Kit to come home early and got Addy’s things ready. We dropped her off at a friend’s house and arrived at the hospital just after 6 p.m.
My contractions were hard, but they weren’t unmanageable. We filled out forms, got hooked up, checked (5 cm), and admitted.
Around 7 p.m. I had four contractions right in a row—with like one minute between them. The nurse came rushing in and pushed me on my left side. She said my baby didn’t like those four contractions in a row (I said, “Well, I didn’t like them either!”), and she gave me an oxygen mask. In about 5 to 10 minutes the baby’s heart rate was back to normal.
We needed to fill out more forms, and then the doctor came in to check me. We’d only really been there about an hour.
The doctor said at 6 centimeters she was going to break my water. Based on my first delivery, I made sure to ask that the epidural would come quickly afterward—I knew the contractions would get ratcheted up to 11 pretty soon. I was assured the anesthesiologist was on the floor and would be there soon.
When the doctor broke my water, she said, “Wow! Look at all this fluid!” A normal amniotic fluid index is between 8 to 18 centimeters; mine was 20. And, it sure felt like a river, but it just kept coming. Even my doctor and nurse were impressed. I visibly watched my tummy deflate. Then I dilated to a 7 within the minute.
The next four to five contractions were hard, but I could breathe through them. Then—just as I predicted—transition came! Yay. My nurse was trying to help me breathe. I was genuinely trying to breathe, but I just couldn’t sometimes. I was a whimpering, whining, moaning mess. I was also really shaky. I kept asking for the epidural and about 30 minutes later he came in.
Kit left for the procedure, and I just whimpered and put my head into my nurses shoulder until my toes started to tingle. Because I was so close to delivery, the doctor didn’t give me an epidural “infusion;” he only gave me drips, so I would still feel my legs but it would take the edge off. If I hadn’t been a VBAC, they might not have even bothered giving me the epidural because I was so close to delivery. But I had to have one in case surgery was needed.

More nurses came in. The doctor struggled a bit to put the internal monitor (more accurate than the belt monitor) on my baby’s head. I didn’t know it at the time, but Isaac had moved. A few minutes earlier his head was in perfect position.
When the doctor was trying to put the internal monitor on the crown of his head (how babies normally come out), she felt his nose presenting. She finally got the internal monitor on his forehead. I didn’t know it right then, but again my baby had moved from the perfect presentation to something that was not ideal.
One nurse kept moving the baby heart rate monitor, trying to find the right one and thinking that his low heart rate was maybe mine, instead of his. His heart rate had dropped and was not coming back up. I couldn’t see the monitor, but I knew more fast-walking nurses probably wasn’t a good thing.
Kit still hadn’t come back in—they didn’t have time to go get him. After about 10 minutes of this, my doctor made the call to do an emergency C-section. She came up to me and said, “I know this isn’t want you wanted, but it’s what we need to do.” I said, “I know; I trust you.”
My doctor had said things like, “Make sure the anesthesiologist doesn’t leave—keep him in the hall,” and, “Now. We need to go, now.” But, I was strangely not nervous or scared for me or my baby. I didn’t really have time to be disappointed. I knew that they were making good decisions, and I really did trust my doctor.
Poor Kit, he left the room for me to get the epidural and 15 minutes later saw them fast-walking my bed down to the OR. A nurse came and told him they were taking me to surgery and to get changed, but then he later found out he couldn’t go in. So he just sat in my empty delivery room waiting.
We got to the OR, and I remember the anesthesiologist saying something like, “Can someone help me get the arm boards?” Then he just went and got them himself. My doctor pinched me hard and asked if I could feel it—yes, I could. Twenty seconds later she pinched again—yes I could feel it. She looked at the anesthesiologist and said, “Is she numb yet? We need to start.” Then he said they were putting me to sleep, and that’s all I remember.
Next thing I know, I woke up, and Kit was holding my hand. Bless him. I could immediately feel the tenderness of my incision. I couldn’t move my legs. My throat hurt from where they had the tube in. I was very sleepy and very cold. My body temperature was 93, so the nurse put a bunch of heated air-blankets on me which I loved. (Seriously, where can I buy some?) I started to talk to Kit. I was a bit hazy, but he said later that I was all there, just running at 10 percent with long pauses and a lot of repetition.
I said, “They put me to sleep.” Pause. “But I didn’t feel anything.” Pause. Looking around. “Where’s the baby?” Seeing the baby. Pause. “Is he OK?”
“Yes, he’s great.”
“What time was he born?” (8:42 p.m.—it was about 10 p.m. when I woke up.) “Do I still have my uterus?”
“Yes, you do.”
“Did you get to go into surgery?”
“No, I had to stay outside.”
“Can I hold the baby?”
“Yes, when you warm up a little bit more.”
“It was OK that I was asleep. Things happened so fast.”
“I know, they did.”
Kit told me that when the baby was born, his one minute APGAR was 2. He was blue and didn’t cry spontaneously. They suctioned him, gave him some pure oxygen, and helped him learn how a breathe a little bit. Then, his five minute APGAR was 8, and his 10 minute APGAR was 9. After those first few minutes, he was vigorous and perfect.
Later my doctor explained more about what happened. She said that we had my VBAC attempt progressing well—all the way until the very end, when everything changed. She said there were several factors that made surgery necessary:
-The baby’s heart rate plummeted in the minutes after my epidural—this was obviously the biggest reason. When she cut into me she saw the umbilical cord coiled down near his head. This is called an occult umbilical prolapse, which basically means that the cord got wedged near his head. As he started to descend into the pelvis, the pressure of his head kinked off the cord, and he wasn’t getting oxygen anymore. It’s a medical emergency and the reason for the rushed surgery. If I had been at home when it happened I wouldn’t have known, and it might have been too late by the time I got to the hospital. The massive amount of fluid I had might have been a factor.
-The baby moved his head and wasn’t presenting well. The doctor felt his nose when trying to put the internal monitor in. Then later when she took him out she said that he was face up at that point but had obviously moved around. (Most babies are face down looking at your back.)
-The baby had his hand up on his face and would have tried to come out with his hand wedged up there. A complex presentation.
So even if the heart rate was fine, we probably would have ended up pushing and having the baby wedged in there again, just like Addy. My doctor said that even though she didn’t feel any notches in my pelvis and everything looked fine, that something about my pelvis makes my babies move at the last second so that they aren’t positioned right.
There were tender mercies associated with being put under general anesthesia. Things were happening so quickly that it would have been stressful to be awake, especially when it took Isaac a few minutes to pink up and cry. I didn’t shake or throw up or have shoulder pain like in my first surgery. I didn’t have to listen to the urgency in the doctor’s voices. I missed the first hour of my son’s life—and I wish I could have been there, but when he was born it was so obvious that he needed to come out right away. And for me, it was more peaceful to wake up and have it over.
In my first delivery, I felt a strong sense of sadness and failure. Everything had gone perfectly, and it felt like I just couldn’t push her out. Something about my body made it so even though I was dilated and pushing, she wouldn’t budge. I had gotten so close and pushed for so long that afterward every time I thought about how it turned out I would start to cry. Everyone else gets to the same point and just pushes out their babies, why couldn’t I?
With Addy, my recovery was normal but not what I wanted and difficult for me emotionally. I was happy to have a baby but physically overwhelmed to be recovering from surgery. I think the hormones didn’t help, but the baby blues were definitely there. I didn’t bond with Addy right away. I didn’t want to hold her; I just wanted to feel better.
This time, I had a completely different emotional response. Because Isaac was in distress, it was obvious that I had to have the surgery to get him out quickly. The factors that made my labor unfavorable were different but still present. I was prepared for the probable surgery, and afterward I haven’t cried once about it! I knew what recovery would feel like. I have been obsessed with Isaac from the first second I held him and wanted him near me always. No signs of baby blues yet.
I’m glad that we tried the VBAC. Even though I didn’t fully deliver my babies vaginally, I labored almost completely (getting my epidural midway through transition both times) with both of them. While incredibly painful, I’m glad that I got to experience labor! I liked knowing what it felt like, I liked managing the pain, and I liked even feeling transition (obviously I didn’t enjoy it in the moment). I liked that I got to feel my water break and be monitored and “waiting” just like everyone else. I liked that we had to wait until I went into labor to go to the hospital (it’s just kind of exciting).
I still have some labor envy of women who labor, push twice and deliver babies. My babies’ birth stories are exactly the same—until the end when they’re not. When you imagine giving birth to your children, you never imagine lying behind a curtain immobile with oxygen in your nose.
Silver linings: My next births will be scheduled C-sections; at least I know that now. No more uncertainty. I’ll never have to wait for the epidural while going through transition labor again! And because my next births won’t be emergencies, Kit can be there, and they won’t be traumatic.
I am truly grateful and blessed to have had a healthy child—he is a miracle to us. We love him and are so happy he is here. I couldn’t imagine what having a second child would be like, but now that he is here I can’t imagine our family without him.
Send us your birth story! Whether you had a home birth, hospital birth, 37-hour labor or emergency C-section, we’d love to read the tale of your little one’s grand entrance. Write up your birth story (click here for tips on getting started) and email it, along with a few photos, to birthstory@pnmag.com. We’ll share it on our Birth Day blog and may even print it in an upcoming issue!