Be my valentine: The birth of Nick

My complications with my son, Nick, first began when I was 11 weeks pregnant last October. Everything started the Friday before fall break, which was also the week of parent/teacher conferences. (I am a third-grade teacher.) I was especially tired this week, and long nights at school meant my diet consisted mostly of snacks I could stash in my desk and fast food between meetings. I was already feeling some nasty side effects of my pregnancy; I had throw-up-in-the-shower-because-you-can’t-make-it-to-the-toilet morning sickness clear into the third trimester, so severe that I eventually needed an anti-nausea medication. That Friday, I was sitting on the couch talking on the phone when I felt a sudden gush of blood. I called the emergency hotline of my OB/GYN’s office, and the triage nurse told me to head straight to the emergency room.
The road ahead
As my husband and I drove to the hospital, I assumed I was having a miscarriage, and I began to think how I would explain this to my 5-year-old. When we got to the ER, a nurse did a quick ultrasound—she was an ER nurse, not a labor and delivery nurse, and explained that the purpose of the ultrasound was not to identify a specific problem, but to determine if the baby had a stable heartbeat. To our immense surprise, the ultrasound showed a squirmy, active fetus whose heartbeat was pounding away like it should. The nurse explained that everything appeared to be normal at the moment, but she told me to make a follow-up with my obstetrician to be safe.
A few days later at the appointment, a more reliable ultrasound showed that I had a subchorionic hematoma, or SH for short. This is essentially when blood gets trapped between the uterus and placenta, causing unexplained bleeding. My doctor was not too concerned about this diagnosis; he explained that cases of SH are relatively common, and usually women will have one incident of sudden bleeding in the first trimester without further issues later in pregnancy. It does cause a slight increase in the risk of miscarriage, so I was placed on pelvic rest (no exercise, no lifting anything heavy) and told to take it easy until my 20-week ultrasound.
The waiting game
For the next few weeks, other than dealing with morning sickness that would not let up, my pregnancy was uneventful. On an early Sunday morning in mid-November, I awoke to find that my pajama bottoms were soaked with blood. Thankfully, my in-laws were in town that weekend; my husband and I left our two sleeping children and headed to the ER, which promptly sent us to labor and delivery. Once again, an ultrasound showed a healthy, growing fetus that was in no obvious distress, but it did show a significant amount of blood in my womb.
Because of the amount of blood evident in the ultrasound, I was admitted to the hospital for observation and had my first appointment with the maternal-fetal medicine doctor (a high-risk pregnancy specialist) the next day. This appointment showed that at 17 weeks into my pregnancy the SH had grown bigger instead of healing. The doctor suspected that it was to blame for the bleeding, and unfortunately there wasn’t really anything that could be done. I was prescribed a week of bed rest to help encourage my body to heal, but I was back in the hospital four days later with another sudden bleeding episode.
This brings us to the important week of December 11. Early that Monday morning, I woke up to discover major bleed No. 4. We repeated what was becoming a familiar pattern for us: Drive to labor and delivery in the middle of the night, then get a quick ultrasound to confirm the baby was not in distress and that I hadn’t begun to dilate—I never did.

The turning point
Nick and I were stumping the doctors. No one could tell us why I was continuing to have the bleeding, and the doctors explained that if it caused me to go into labor at 21 weeks, Nick would be too premature to survive. There was nothing the doctors could do at the moment other than to hope for the best. We were given a 50 percent chance of making it to 32 weeks, were told to plan for long-term hospitalization due to bleeding, and that in order to try and stay pregnant as long as I could, I would need to be on bed rest for the remainder of my pregnancy.
The most important thing to come out of that scary time in the hospital was that my doctors were more or less expecting Nick to be born prematurely, so shortly after Christmas, I received my first round of steroid injections to help speed up Nick’s lung development. This would prove to be a massive blessing during his time in the NICU.
Approximately eight days before Nick was born, my birth story gets really weird. I had a prescheduled ultrasound and appointment with my doctor, and the ultrasound showed the SH was completely gone. Vanished. It seemed as though bed rest had finally allowed my body to heal, and the doctor said there was nothing on my ultrasound that would indicate I wouldn’t have a normal, full-term pregnancy. It “wasn’t quite in the miracle category, but it was close,” he said.
A few days later I woke up in the middle of the night with an intense pain in the lower left side of my back. It felt as though someone was twisting a knife deep in my side. I called and spoke to an on-call doctor who told me to take Tylenol, drink a bottle of water and call back if the pain didn’t stop. I followed her instructions and was able to go back to sleep for another hour or so, but the pain eventually returned. I headed to the hospital and was strapped to a monitor to check for contractions. The monitor showed I was indeed having contractions, but they were anywhere from 4 to 10 minutes apart (re: I was not in labor). By that point, the pain in my back had dulled to more of an ache than a sharp pain. I was sent home and told to come back if the contractions became more frequent or more painful.
For the rest of the day, I continued to have uncomfortable back pain and sporadic contractions. Around 7 p.m. the bleeding started, and back to the hospital we went. This time, I was having consistent, labor-like contractions and was admitted again and given a second round of steroid injections. The next day, at 30 weeks’ gestation, I was told I finally had too many bleeding episodes and would need to spend the remainder of my pregnancy in the hospital.
The final stretch
The day before my son was born, I had another appointment that changed my situation significantly. An ultrasound revealed that the pain I had most recently was a mild placental abruption, which is where the placenta begins to separate from the uterus. This happens in the final stages of delivery, but when it happens prematurely, it becomes a big deal, as the placenta is the baby’s lifeline to the mother. I also had an enormous blood clot attached to my umbilical cord, and there was blood in the amniotic fluid. In summary, things were going south very quickly.
That night, a nurse practitioner from the NICU met with us about the possible risk of having a baby born at 30 weeks. She explained that the doctors would not induce labor unless Nick and I showed signs of distress because a crucial part of a baby’s lungs do not develop until 32 weeks’ gestation. The plan was to try our best and hang on for two more weeks.
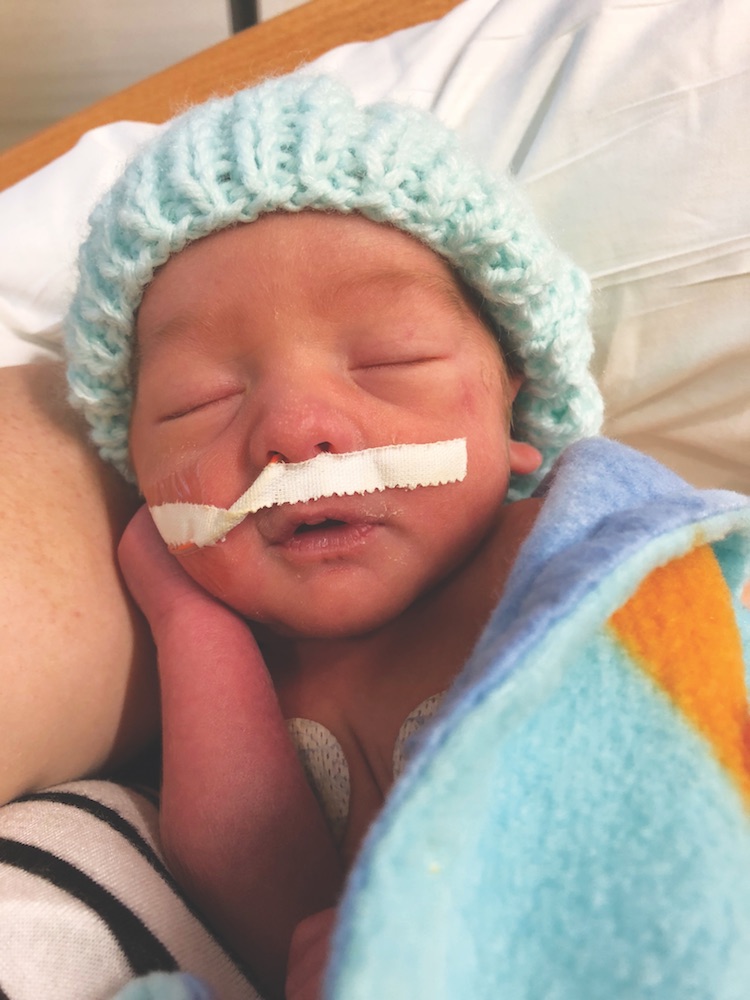
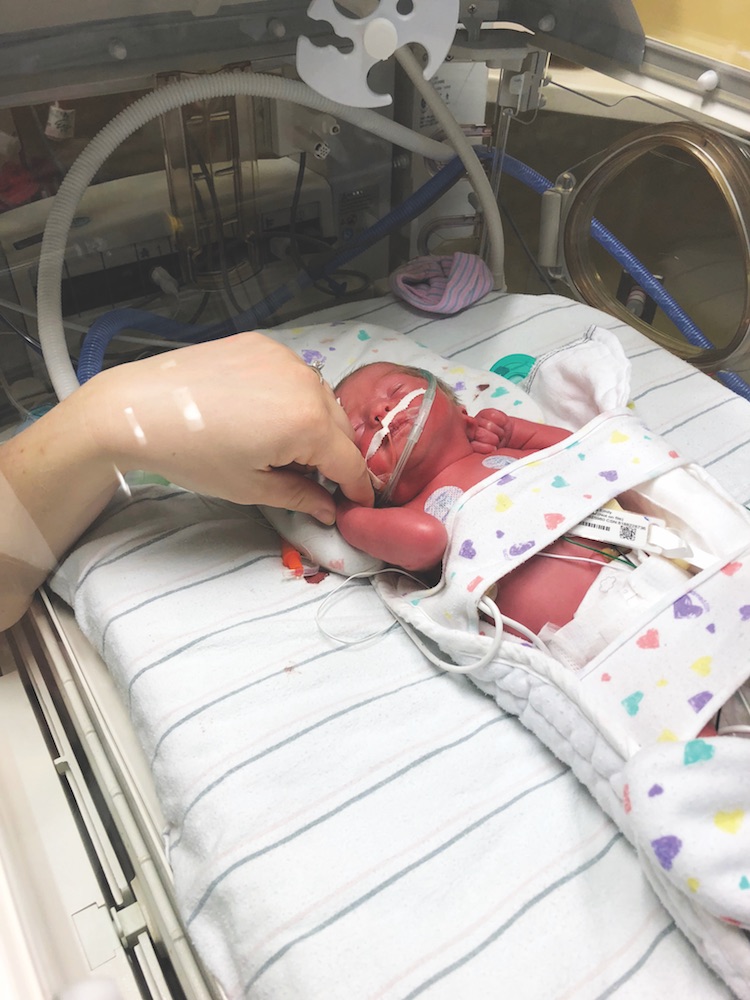
Around 9:00 a.m. on Valentine’s Day it was becoming obvious that my body could no longer stay pregnant. I signed papers consenting to a possible C-section and was told not to eat or drink anything in case I needed to be rushed to surgery. Finally, at 10:30 that morning, the doctor made the call to take the baby out right away. After that, things moved rapidly. As I was being prepped for surgery, my bleeding became severe, and I was rushed to the O.R. The anesthesiologist administered the spinal block, and the C-section began at 10:50 a.m. Nick joined the world at 11:02 a.m. and was immediately handed to the NICU staff standing by. We were told that he was strong and was big for a baby born 10 weeks prematurely, weighing 4 pounds at birth. We were able to see him briefly as he was wheeled past us on his way to his new home in the NICU, where he spent the following 53 days. Afterward, the obstetrician told us the surgery had gone well and the abruption had become significant. I spent a few hours in recovery before we were taken to see Nick. I was not able to hold him, but I was able to touch his hand through the side of his Isolette.
It is humbling and overwhelming to think how lucky we are, and how differently things could be today if Nick was not born exactly when he was. During his stay in the NICU, Nick was always healthy and never had any major health concerns. We know there are many mothers who suffer placental abruptions and never get to bring their baby home. Nick is a true miracle baby, and I am so thankful every day for the doctors and nurses who gave us the opportunity to raise him and watch him grow.

Send us your birth story! Whether you had a home birth, hospital birth, 37-hour labor or emergency C-section, we’d love to read the tale of your little one’s grand entrance. Write up your birth story (click here for tips on getting started) and email it, along with a few photos, to birthstory@pnmag.com. We’ll share it on our website and may even print it in an upcoming issue!







